Using a Sylff Leadership Initiatives award, Shephy Elisha Oduor (University of Nairobi, 2021–22) organized and implemented a two-day youth empowerment workshop in Nairobi for over 200 young women and adolescent girls to explore the intersection of digital literacy, online safety, and gender-based violence prevention in urban Kenya.
* * *
Technology is a useful servant but a dangerous master.
—Christian Lous Lange
Over the past decade, digital technology has reshaped the social landscape for young people across the globe. In Kenya, the rapid growth of smartphone ownership and internet connectivity has dramatically transformed how young people access information, communicate with peers, and pursue opportunities. Social media platforms have become powerful spaces for education, entrepreneurship, creativity, and civic engagement. For many young people, digital platforms provide opportunities that were previously unimaginable. Students can now access educational resources, build networks across borders, and participate in global conversations without leaving their communities.
Yet these expanding digital opportunities also come with significant challenges. As digital access grows, so too does exposure of young users to online threats, such as manipulation, harassment, and exploitation. Online grooming, sextortion, phishing scams, impersonation schemes, cyberbullying, and digital stalking have become widespread concerns. For adolescent girls and young women, these risks are often compounded by social and economic vulnerabilities. In many urban informal settlements, digital literacy education has not kept pace with the rapid adoption of smartphones and social media. As a result, many young women enter digital spaces without adequate preparation to identify or respond to online manipulation.
Recent national discussions on gender-based violence and femicide in Kenya have highlighted the need to examine how online interactions can intersect with real-world harm. In several reported cases, online deception or manipulation has preceded incidents of exploitation or violence. These realities underscore the need for proactive education that equips young people with practical knowledge about digital safety while strengthening community awareness of online exploitation.
It was within this broader social and technological context that the workshop on Navigating the Digital Age: Raising Awareness on Social Media Risks and Femicide Awareness was conceptualized. The initiative sought to equip young women and girls with practical skills to protect themselves in digital environments while also fostering awareness about the connection between online manipulation and gender-based violence. By combining digital literacy training with conversations on femicide prevention, the workshop aimed to empower participants to navigate digital spaces with greater awareness, confidence, and responsibility.
More than 200 participants attended the event, including primary beneficiaries as well as adolescent girls aged 16 and 17. Their presence reflected the growing urgency of introducing digital safety education early, as young people begin engaging with social media platforms during adolescence.
From the moment participants arrived at the venue, the atmosphere was intentionally designed to communicate solidarity and shared purpose. Each participant received a pink awareness T-shirt and wristband carrying the message: “Stay Safe Online: Navigating the Digital Age—Fight Against Femicide.” Participants were also provided with digital safety manuals and informational guides outlining available reporting mechanisms for online abuse. These resources ensured that the knowledge shared during the workshop could continue to serve participants long after the event concluded.
Building Awareness Through Dialogue

Participants gather in Nairobi for the two-day digital safety and femicide awareness workshop, demonstrating youth solidarity and shared commitment to safer digital spaces.
The workshop opened with a plenary session designed to create space for honest dialogue about digital experiences among young women. Facilitators guided discussions exploring how digital interactions—often beginning with seemingly harmless communication—can sometimes evolve into manipulation or coercion. Participants examined real-life scenarios involving fake job advertisements, romantic deception schemes, identity theft, and online blackmail. These examples resonated strongly because they reflected situations that many young people had encountered when navigating social media platforms.
Through guided conversations, participants reflected on how trust is established in digital environments and how that trust can sometimes be exploited. They identified warning signs such as requests for private images, emotional pressure, financial demands, and attempts to isolate individuals from their support networks. These discussions were particularly impactful because they allowed participants to learn from each other’s experiences while developing a deeper understanding of digital risk.
Practical Digital Safety Skills
A key strength of the workshop was its emphasis on practical learning rather than theoretical discussion alone. ICT professionals facilitated interactive sessions where participants conducted live digital safety audits using their smartphones. They learned how to review privacy settings across their social media accounts, activate two-factor authentication, strengthen password security, and disable unnecessary location-sharing features.
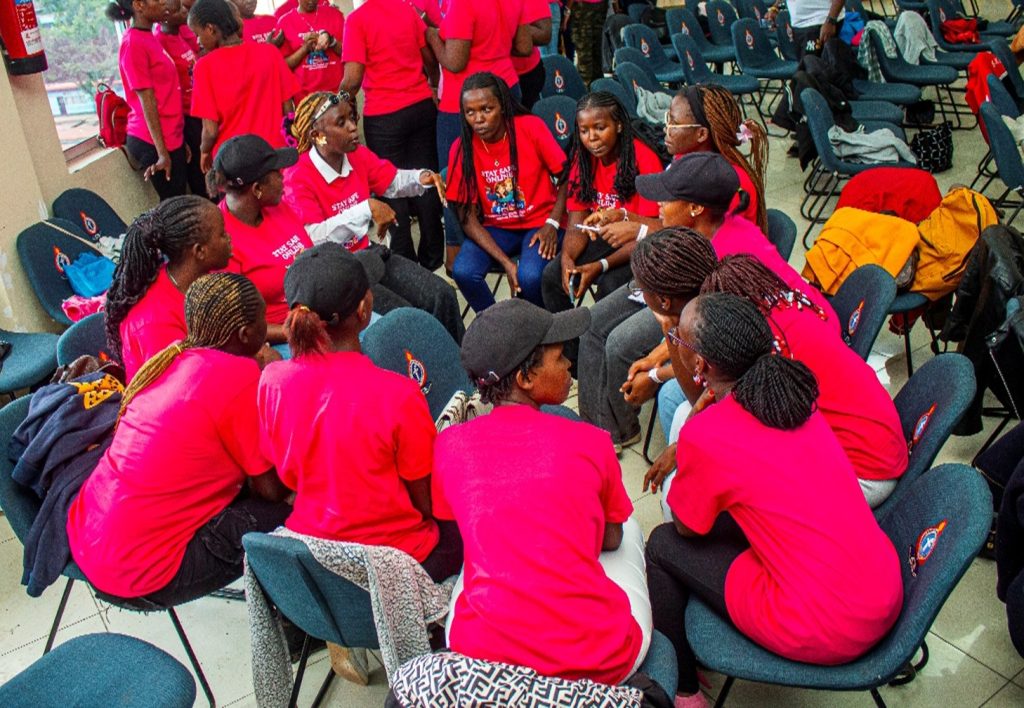
Participants conduct digital safety audits by reviewing privacy settings and strengthening online protection during group discussions.
For many participants, this exercise revealed previously unnoticed vulnerabilities. Several discovered that their social media profiles were publicly accessible, exposing personal details such as phone numbers, school locations, and daily routines. Facilitators explained how cybercriminals and online predators often collect publicly available information to build trust with potential victims. Understanding these tactics helped participants recognize how seemingly harmless online behavior can sometimes create pathways for manipulation. By the end of the session, participants expressed significantly greater confidence in managing their digital identities and protecting themselves online.
Leadership Through Knowledge: Miss Digital Safety 2026
A distinctive feature of the workshop was the selection of Miss Digital Safety 2026, an initiative designed to recognize leadership in digital safety advocacy. Unlike traditional pageantry, the recognition focused on knowledge, communication skills, and community engagement rather than physical appearance. Participants were evaluated based on their understanding of digital safety principles and their ability to communicate prevention strategies clearly.

Miss Digital Safety 2026, seated, with mentors and other finalists. The winner was recognized for leadership in promoting responsible online behavior and digital safety awareness.
The initiative emphasized that digital literacy itself is a form of empowerment. By recognizing knowledge-based leadership, the program encouraged participants to view themselves as advocates capable of promoting safer digital practices within their communities. The crowned ambassador committed to conducting peer awareness sessions among fellow youth, ensuring that the knowledge gained during the workshop would continue to spread beyond the event.
A Multi-Stakeholder Approach to Digital Safety
One of the strengths of the Navigating the Digital Age initiative was its integrated and collaborative approach. Rather than focusing solely on awareness campaigns, the workshop combined several complementary strategies designed to address digital safety from multiple perspectives.
Participants engaged in practical training sessions addressing online scams, digital grooming, and phishing tactics. Expert facilitators provided insights on the legal frameworks governing cybercrime, technological safeguards for digital security, and the broader social implications of online exploitation.
The workshop also emphasized peer mentorship and community engagement. By encouraging participants to share knowledge within their peer networks, the program sought to cultivate a culture of digital responsibility among young people themselves. Community leaders, educators, and digital security experts participated as mentors and facilitators throughout the program. Their involvement reinforced the idea that protecting young people in digital spaces requires cooperation between families, schools, community organizations, and policymakers.
Measuring Impact and Sustaining the Initiative

Participants pose with Professor Susan Chepkonga, a workshop facilitator, and the author at the close of the workshop, united in their commitment to advancing digital safety and femicide prevention.
As the conversations around digital safety continue to gain urgency, initiatives such as Navigating the Digital Age are increasingly recognized as timely responses to emerging social challenges. The program demonstrated how digital safety education can be strengthened when practical training, expert guidance, peer mentorship, and community engagement are combined within a single learning platform. By addressing both the technical and social dimensions of online risk, the workshop created a holistic approach to digital resilience among young participants.
At the same time, the initiative recognizes the importance of systematically evaluating its long-term effectiveness. Future phases of the program will therefore incorporate structured evaluation strategies designed to assess both immediate learning outcomes and sustained community impact.
These will include post-workshop surveys, structured participant feedback mechanisms, and tracking of peer outreach activities conducted by participants after the training. Such tools will provide valuable insights into how knowledge gained during the workshop spreads within communities and influences digital behavior over time. The aims of strengthening monitoring and evaluation frameworks are not only to refine future workshops but also to contribute evidence-based insights that can inform broader, digital-safety education programs.
Reflection: Protecting Dignity in a Digital World
The Navigating the Digital Age initiative highlights an important reality of contemporary life: digital literacy has become inseparable from personal safety. When young women understand how to safeguard their digital identities, recognize manipulation early, and access support systems when needed, they strengthen not only their own safety but also the resilience of their communities.

A digital safety advocate shares experiences and insights during the workshop.
In a world where technology increasingly shapes human relationships, the challenge is not simply to expand access to digital tools but to ensure that young people are equipped with the knowledge and confidence to use them responsibly.
Ultimately, building safer digital environments depends on the collective efforts of informed individuals, supportive communities, and young leaders committed to protecting dignity in both online and offline spaces.